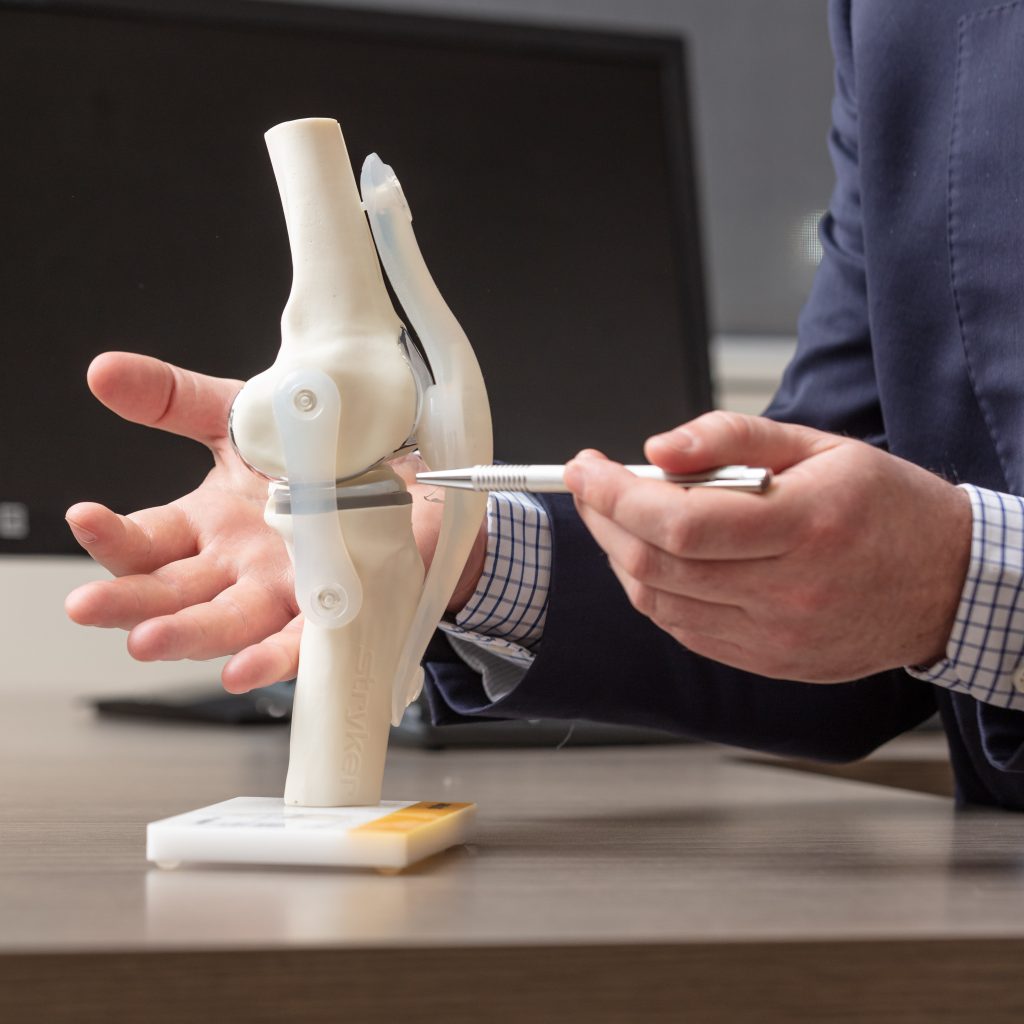
What Happens If Your Kneecap (Patella) Is Unstable? Patella Dislocation & Patellar Instability Explained
Patella dislocation is a common traumatic knee injury where the kneecap (patella) slides out of its normal trochlear groove on the femur. While many first-time dislocations settle with conservative care, recurrent episodes or a persistent feeling of instability often indicate patellar instability that requires specialist evaluation.
Understanding patella dislocation and patellar instability helps ensure timely assessment and the most appropriate treatment to protect knee cartilage and prevent long-term issues such as early osteoarthritis.
Why the Kneecap Can Become Unstable
The patella sits in a shallow groove at the front of the femur and is stabilised by ligaments (particularly the medial patellofemoral ligament – MPFL), muscles, and the bony anatomy of the joint. It is designed to track smoothly during knee movement.
Dislocations typically occur laterally (outward) during twisting injuries, sudden direction changes, or direct impact, often tearing the MPFL and sometimes damaging the cartilage surfaces.
Common contributing factors include:
- Shallow or flat trochlear groove (trochlear dysplasia)
- High-riding patella (patella alta)
- Ligamentous laxity or generalised hypermobility
- Muscle imbalance, particularly of the quadriceps (VMO)
- Alignment variations such as increased Q-angle or tibial tubercle malposition
These anatomical features can make the kneecap more prone to instability, even with relatively minor forces over time.
Initial Management of a First-Time Patella Dislocation
Most first-time dislocations are managed non-operatively. Treatment usually starts with prompt reduction of the patella (it often returns spontaneously or is gently guided back), followed by short-term splinting or bracing, pain management, and early physiotherapy.
Many patients recover well after a single episode with structured rehabilitation focusing on quadriceps strength, hip stability, and patellar tracking. However, the risk of recurrence remains notable, particularly in younger or more active individuals.
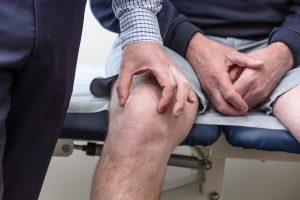
Investigations for Patellar Instability
Following a dislocation, imaging is important to assess for associated injuries. This commonly includes:
- Plain X-rays to evaluate alignment and rule out fractures or loose bone fragments
- MRI scan to identify MPFL tears, cartilage damage, osteochondral loose bodies, and underlying anatomical risk factors
Early detection of significant cartilage injury or loose bodies may allow for timely intervention to minimise future joint wear.
Symptoms of Patellar Instability
Patients often report:
- A sensation that the kneecap is slipping, shifting, or about to give way
- Pain at the front or inner aspect of the knee
- Swelling after episodes of instability
- Recurrent dislocations that occur with progressively less force
- Difficulty with twisting, pivoting, or changing direction during sports or daily activities
- Knee buckling or giving way
Repeated instability increases the risk of cartilage damage and early patellofemoral arthritis.
Treatment Options for Patellar Instability
Treatment is individualised based on the frequency of dislocations, degree of instability, and any underlying anatomical issues. Dr Woodbridge takes a holistic approach, considering each patient’s lifestyle and goals.
Non-surgical options (often suitable for first-time dislocations):
- Targeted physiotherapy to strengthen the quadriceps, improve patellar tracking, and enhance hip and core stability
- Activity modification and temporary use of a patellar stabilising brace
- Gradual return to sport with guidance
Surgical stabilisation is typically considered for recurrent dislocations or persistent instability despite physiotherapy. Procedures are tailored and often combined:
- MPFL reconstruction — using a hamstring tendon graft to restore the torn inner stabilising ligament (the most common procedure)
- Tibial tubercle osteotomy (medialisation or distalisation) to correct alignment or patella alta
- Arthroscopic procedures such as lateral release/lengthening or chondroplasty for cartilage issues
- Trochleoplasty in selected cases of severe trochlear dysplasia
Rehabilitation after surgery is guided and usually allows return to pivoting sports around 4–6 months, depending on individual progress.
Expert Assessment for Kneecap Instability in Sydney, Taree & Forster
If you have suffered a patella dislocation, feel ongoing instability in your kneecap, or experience recurrent slipping or giving way, prompt specialist review is recommended.
Dr Adam Woodbridge, a fellowship-trained orthopaedic surgeon with a background in physiotherapy, provides detailed assessment and personalised treatment planning for patellar instability and all knee conditions. He offers consultations and surgical services in Sydney (multiple locations including Bella Vista, Chatswood and Inner West), as well as Taree (Mayo Specialist Centre) and Forster (Dolphin Specialist Suites) for the convenience of patients on the Mid North Coast.

Contact Dr Woodbridge’s rooms today on 8785 5422 to book an appointment and discuss the best options for your knee.